The following is directly from Ethan's Facebook Group Page;
A blog that was used to keep everyone up to date on his status.
There may be typos, there may be some areas not 100% medically correct.
However, these are his father's words, the way he coped, and his
understanding of how things were going. To preserve the original
moment, no updates or modifications were made to the content, hindsight or not.
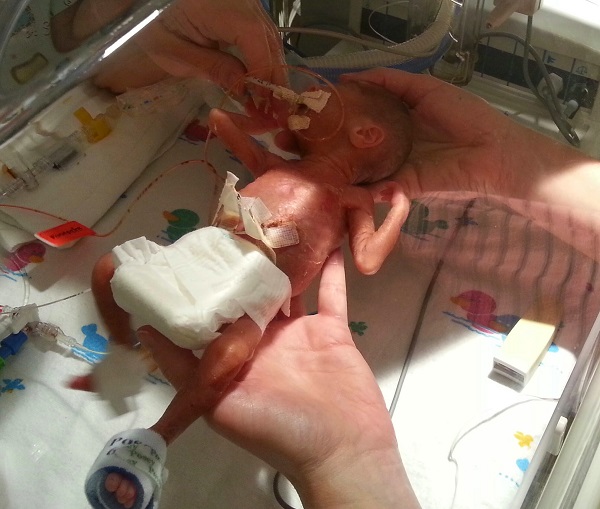
On Friday, Prudence was admitted with preterm labor contractions... Doctors did everything but Ethan was born this morning, only 23 weeks 1 day, at 6:29am. He is 12 inches and 1 pound 1 oz. He's going to be a fighter. We ask for thoughts and prayers. Even if you skim this... Please take even a moment to think of Ethan and wish him the strength to fight this. Prudence is fine... We just need the thoughts and prayers for our sweet boy, Ethan. Thank you.
Ethan got through the night fine... his breathing and lungs appear to be good. They did give Prudence steroids before his birth so that definitely helped him. His sugar is a bit high so they started on insulin. Nothing "bad" since that is pretty normal at this age... liver and pancreas just aren't developed enough yet. He may require a blood transfusion as well... again not an "if" but more of a "when" since he is so little.... but still common for prem babies anyway. So point is, nothing out of the ordinary. These first couple weeks are incredibly delicate and fragile... So each day, each moment, is a bit scary for us but we are doing everything we can for the little man. We know there will be setbacks... sometimes that 1 step forward and 2 steps back.. all we can do is continue to pray and hope he fights through everything. Prudence is doing fine.. there was some fluid in her lungs, most likely from the magnesium (given to her to protect Ethan's brain) but that's mainly cleared up. She should be able to leave the hospital tomorrow. Plans are to stay with my brother in Battle Creek and then make our regular visits to the Bronson NICU here in Kalamazoo.
Not a whole lot... No news is good news if you ask me. He has lost about 1 oz so he's right at 1 pound. The nurse said they actually like babies to lose an initial ~10% of their birth weight at first... even the tiny little guys, so no worries there. He did get his blood transfusion last night... seems to have gone OK. As you may have seen in the video Prudence posted, he's active and looking good. He is starting to open his right eye a bit too... You can kind of see that in the video as well.
They also removed the biliblanket (blue light) which helps with any bruising (higher and common for such a preemie) and lack of red blood cells. Basically, his red blood cell count has improved, due to the blanket and transfusion he received.
His blood sugar is still higher than ideal but under control and coming down from where it initially was. They brought down the insulin slightly (was 0.1 unit/kg/hour and now 0.06).
The Respiratory therapist was very please with how he is doing. They are always adjusting his oxygen volume... We all breathe 21% oxygen and he is constantly around 21% with sometimes a bump up when they are really working with him. Point is, he's doing fantastic in that respect. It appears the steroids that Prudence received over the weekend (aimed to help his lungs) are doing their job.
Prudence's breathing is better now too (she still had a slight crackle in her lungs) but that's pretty much gone. She is being discharged today.
Ethan had another good night. They are still playing with his insulin but that's expected. It's all sort of a catch 22 to make him the right cocktail... He needs the sugar they give but obviously more sugar raises his blood sugar. There are several other examples like this but they are finding that perfect mix and he has been responding well to things.
The doctor did say that he will start giving some of Pru's breast milk today which is also awesome... He can get some of those natural nutrients and good bacteria, especially in his upper GI. Great news there. Additionally they will reduce his breathing support a bit to give him an opportunity to do it on his own... He's been showing that ability so it's a matter of tweaking that... Bump it up and down as needed but great to know he's showing such progress and maturity with his breathing.
They typically do his brain scan (check for bleeding) after 7 days but want to do it tonight. The doctor stressed several times that there is no concern for them wanting to do it early. She actually sounded like an impatient parent that just "needed to know." so they'll do it tonight. Big big prayers for him tonight. He will still get another one after 7 days...they typically do them literally middle of the night so results maybe tomorrow noon. Longest 24 hours coming up. This is really the only other major hurdle.... Obviously a lot more to go but this would be a huuuuuge step to come back normal. Thank you all for the continuous thoughts and prayers. #EthanStrong
His scan seemed to go well... Dr is not concerned since the radiologist report said there "could maybe might" be a small amount of blood. Hard to tell since it "could" exist in areas next to other vessels that show up the same as blood would show... Point is, nothing major or obvious was seen hence the use of "maybe could be."
More details to come later this afternoon.
A more thorough update...
Once again he had a good night... no issues whatsoever. The biggest event of his night was the ultrasound for his brain. This came back pretty much normal. The radiologist could not see anything definitive that was wrong. There might have been a small amount of bleeding but again, could not really be "proved." The doctor, who read the results, was not concerned. They are canceling his initial, planned, 7 day ultrasound (Sunday night) and just doing it again 7 days from today. Frankly, that says a lot. She is not taking any action, he looks great, and she sees no reason to do another ultrasound until a week from now. To not be a pessimist, things still happen but he's been showing all great signs (platelets steady and are not dropping and he has great color). Additionally, she did say (knock on wood) that the major hemorrhaging typically happens by now. Again... knock on wood... pray pray pray pray pray.
His blood sugar has been dropping a lot and so has his dose of insulin. The fact that he does not require so much insulin and the blood sugar is coming down to normal levels tells me that maybe that his liver and pancreas are probably starting to do their job. The latter is my assessment, but hey, that makes sense considering he needed the insulin because they were underdeveloped. It'll still be a game with the insulin but really Pru and I could "care less" if that's the only problem he has long-term. We say that to the doctors and even then they reassure us that his current insulin needs mean nothing for his future (in a good way). He is back to using the biliblanket. He is slightly jaundice and has bruising. The fact that he is back on it doesn't really mean much... very normal. We are told that it's not uncommon for even full term babies to sometimes go home with them. So the fact that this 23 week dude was on it for only 2 days and then off was almost ridiculously rare.
The only "bad news" of the day is concerning but at the same time not abnormal for this little man. They do hear a heart mumur. They believe it is a PDA (Patent Ductus Arteriosus). There is this small valve that should close (sometimes takes a couple days after typical birth) to allow the lungs to oxygenate the blood. Otherwise, if it stays open, then you have deoxygenated blood flowing through the body without getting oxygenated by the lungs first. Make sense? Ha. If not, google it. ;) The doctor is NOT worried about this murmur. It is expected and should close on its own. She mentioned an EKG and even meds that would help to close it... To prove she is really not as concerned, and is confident it will close on its own, she sees no need to do the EKG just yet. They have lowered his tidal volume (TV) from 2.9 to 2.8 yesterday and now to 2.6. The closer this number gets to 2, the less the machine is doing the breathing for him. She was hoping this number would've been down sooner. But because of that PDA, she is suspecting that is the reason for the higher TV at this stage. If you re-read this paragraph, it really does make sense. Basically, PDA needs to close up, that increases the amount of oxygenated blood through his body, decreases the amount of machine support and therefore decreases the amount of stress/scaring to his lungs from the machine.
His skin is coming in nicely... almost "complete" and the little guy even grew some eye lashes. The cutest freaking eyelashes ever....
Even with the above good and bad at the end of the day he is stable... like... literally... stable numbers all around and just relaxing.... so that's really the most important thing. At this point... exhale a little, continue to pray, and hope he continues this awesome course of outweighing the downs with so many ups. #EthanStrong
Ethan continues to do great. He is back to 1 pound and 1 ounce. His Tidal Volume (TV) has been reduced to 2.3 which is the right direction. I've asked about his heart murmur and when they want to see it get better but there isn't really any concern. If they hit a point of having trouble reducing his breathing support, then they may look at the CPA issue more closely. But at this point, they are able to reduce the machine support so let the CPA figure itself out. As many folks posted, it happened with their baby, its not uncommon, and tends to resolve itself.
He is completely off the insulin, at the moment. Last night when we left, they stopped it since his sugar was too low. Since then, it's gone back up to the normal range and has maintained. As I said yesterday, "Dr DVO's" assessment seems to imply maturity from his liver and pancreas since he doesn't require the insulin at this time.
The biliblanket has been removed... I would not be surprised to see it back (again, not a bad thing) but just further indication that this little man's levels continue to be where they should.
He did have an x-ray last night to see how his breathing tube is placed and the lines to him umbilical cord are looking... all seems OK. They'd like to remove the lines to his umbilical cord within the next week... at which point they put in a PICC line. It's a catheter and similar to your "typical IV" but just a more long-term solution.
He is off his antibiotics and shifting to just one bag of fluid for his nutrients... he was on several to try and make that perfect cocktail to keep him balanced. Sorry to let you guys down... I feel like I should have known more details about each fluid he was getting but I just haven't gotten that far.... yet. ;) I think the main thing here is the visual.... He had 6 machines with 6 different fluids/meds hitting him. We've basically cut that in half today so just nice to see less machines/bags keeping him going.
They are increasing the frequency of milk... was getting 1 CC (mL) every 6 hours and now it will be every 3 hours. Great news considering he is showing good toleration to that!
Prudence has a knack for asking each day "What can I worry about next?" The response from the doctor was just trying to get him off the ventilator and on a CPAP. The smallest CPAP they have is too big... the prongs that go in to his nose would not fit. They can rig something up so as long as he continues to lower his machine support, we can get him on the CPAP soon.
As you see, continues to do well and not much new news. I suppose this is proof of my ability to ramble a couple small points.
Prudence and I will try and get out today versus sitting in his room pretty much 10 hours straight. It's tough since we feel that separation anxiety but we are trying to make sure and take care of ourselves the best we can. I think last night was the first night we actually slept almost the whole time and for a good 8 hours. Much needed.
Thank you all for the continued support. #EthanStrong
Ethan had a "fair night." There wasn't anything bad but it was just OK. His heart rate and oxygen saturation have been a little erratic... Heart rate may be 160s then suddenly in the 50s for about 10 seconds... but long enough for nurses to come running in before it jumps back up on its own. The oxygen saturation would do the same thing. We are being told that it is OK and normal but you can imagine our own hearts sinking when he does that. It's not often but has happened a handful of times. I think it mainly has to do with him being an extreme preemie but mainly that *he* is starting to do a lot of the work vs. the machine.
They are giving him another transfusion as we speak. The doctor is confident that it will help him with his current needs and also may hep with the weening of the ventilation support. I think they maybe rushed him a bit considering they reduced his tidal volume from 2.9 to 2.8 on Friday and then Saturday from 2.8 to 2.1. He's closely monitored by them taking his blood gases (a measure of oxygenation and ventilation) so they adjust based on that. His tidal volume is back up to 2.3. Again, nothing really bad since net, he is improving. They want his tidal volume to be about 4cc/kg... he is less than half a kg so around 2 is ideal. But at the same time, as he gains weight he may very well "grow in to" his tidal volume since that ideal number is based on weight. Once we get the TV down to an appropriate value, then they will work on his Rate. The Rate is how many breaths he gets per minute by the machine. He should be getting around 60 (being so young, his body is working extra hard) and the machine is giving him all 60. So once we can an appropriate **volume* of breaths he gets (the TV) then they will reduce his Rate (the quantity/minute). Ideally, you want the rate around 40... meaning if he should breathe 60 times/minute, the machine does 40 and he does 20 on his own. At the end of the day, we are moving in the right direction. Yes, the doctor wants to see more progress to get him off the machine but not really in a danger zone at this time.
I am scared to say it but the doctor even said we're so close to that point of being able to say "we're in the clear." I almost tremble typing that but this whole breathing thing is truly the next major hurdle. She just wants him off the machine. Even if he goes off for a bit but has to go back on it temporarily, that's OK. We just want him off even for a moment. So if I had to pick one thing to be very pointed.... his lungs have to start working on their own without machine support. Breathing support is one thing but machine doing all the work (current state) is another.
His blood sugar is still good... no more insulin. They will take him off the breast milk today while he gets the transfusion. That is standard protocol and would plan to resume the break milk tomorrow. The doctor was extremely excited that his electrolytes are consistently perfect. Another good sign.
He is able to open both eyes wide enough for you to see them... will try to get a picture later. The lights are often dim, except during active nurse care, so we like to keep them that way as much as possible. Maybe during the next care session, we can snap a pic.
His only fluids that he is getting now are TPN (Total Parenteral Nutrition), basically all his nutrients, and caffeine. On hold at the moment is the breast milk and lipids. The lipids are fat for him... they put them on hold because his triglycerides are a bit elevated. No real concern but that's given on an on/off basis. Just tryin' to get some fat on him, safely.
She still hears the heart murmur... didn't really expect it to go away overnight but at the same time, we would like it to go away. If you recall from an earlier post, the PDA (Patent Ductus Arteriosus) being open could be the root cause to still requiring so much machine. If tomorrow it still appears we need a lot of the machine, then they may order the EKG to confirm the heart "problem" is the PDA, as she suspects, and nothing else. If it's the PDA then we she may start to medicate which is ibuprofen or indomethacin. Since the idea is to close the PDA, there is a side effect of closing other vessels such as those to his kidneys. Should they start to notice that, they can back off and things should "back to normal." Hopefully I am just explaining things here that become a moot point. The current transfusion he is getting could in fact help overall, including closing of that PDA. So, long point short... hope the transfusion is an overachiever and we don't have to worry about the EKG or meds to close the suspected PDA.
Overall, he continues to do just fine and nothing that has been unexpected. I think we've just been a bit spoiled lately with him being a rock star... so the fact that he has been slightly erratic the last 24 hours with his heart rate and oxygen saturation has us feeling a little down. As I said, we've been spoiled. But hey, at least these blips are expected and he has still done NOTHING considered serious or truly losing sleep over.
Continuing to pray and hope for our sweet boy. #EthanStrong
Happy one week birthday to our sweet boy! Initial briefing is a great night, nothing big to report. A more comprehensive update coming later this afternoon. I'm going to start working today with planned visits. The distraction should help. Pru is off all week and will be with him. Detailed update later after I hear from the doctor.
Quick update and I will follow up this evening with more details. The doctor has ordered an echocardiogram (not EKG as I mistakenly said previously). The echo is ordered to prove that he has the PDA. They cannot give the meds to treat the PDA until they prove that is what is causing the murmur. The docs still feel certain that the murmur is the PDA... so again, just following protocol by proving it.
To treat the PDA, they would give him ibuprofen or indomethacin. Both can have an effect of thinning the blood. The other day when they did his brain scan, and told us "could/maybe..." we learned today that the results were actually "could be a grade 2." Prudence and I were a little annoyed they didn't tell us the "grade 2" part but at the same time I believe the doc was trying to not worry us since it was not definite. Today, they have ordered another brain scan. If there is bleeding and it is getting worse, then the indomethacin is NOT good.... If it's still the "maybe/could be" then no worries. So how about we just hope a result of, "we see NOTHING."
So... Echo to confirm the PDA. Brain scan to ensure brain bleeding isn't more serious so they provide the meds to treat the PDA.
Now you know why this is a quick update and more details to follow later. His brain scan is scheduled for 2:30PM EST. Echo is most likely later this evening.... I'll keep you all updated as we learn more about results. #EthanStrong
Echo confirmed a large PDA... No worries that it's "large" as they expect it to be.
The brain scan came back showing a possible small clot (apparently this also existed last week but never told) and maybe the subtle bleeding but otherwise normal. Last week they said "could be grade 2" and today they don't even mention that it could be. So I see this as a bit of an improvement. They will start the medication, indomethacin, today that should help close up the PDA.
Sorry, about the lack of a comprehensive update last night... We got a bit exhausted. I'm sure you understand. ;-)
Monday was a bit awkward. We had a new doctor that is good at what he does but lacks the personality. He is just very direct and to the point without much opportunity to ask further questions. Maybe that's why I wasn't motivated to post more info?
This morning, our regular doctor was back so already Pru and I feel like today is a "good day." They have reduced his volume intake in prep for the indomethacin. As mentioned in previous posts, they suspected the PDA (Patent Ductur Arteriosus) but needed an echocardiogram to prove it. It did prove a "Large PDA." The fact that it is large or not means nothing really... they did expect it to be large since he is so young. Full term babies can have them but also their respiratory is much more mature so it's OK. Because Ethan's immature all around, they would like to see this close, even slightly, as that would help his respiratory. In order to treat it, they give indomethacin and a side effect would be bleeding and closing vessels that go to his kidneys. They did the brain scan yesterday to determine if there was significant bleeding already. There was not. They did see a small clot but it was not near any neural vessels (I believe that's how she called it) so really it's of no concern. The clot was there last week... seems about the same but they expect it to go away on its own and not batting an eye. Last week they said, "could be grade 2" bleeding and this go around was "maybe subtle but otherwise normal." With that said, no bleeding, if any, to worry about so they could carry on with his indomethacin therapy. To monitor his kidneys, they take blood and check for his creatinine levels. In a nutshell, this is a measure of his kidney function. So if those vessels close up, they will be able to tell from these tests. Should they close, it's just a matter of stopping the indomethacin.
The indomethacin is given in 3 doses over 36 hours... he had his first dose Monday at 10PM EST. Typically you would hope if the murmur goes away (implying PDA closed) within 24-48 hours of his final dose and then he is done with a first round... so should be gone by Thursday-ish. However, the doctor did say that since he is so small, in a way, she does not expect it to go away with one round. They can do a second round and she would want to do it immediately following... so in a way he will get a 72 treatment (6 total doses). Of course, if they notice the murmur is gone at any point, then they will stop it.
Regardless if they cannot fully close the PDA now, they are still trying to get him on to a CPAP. They do not expect him to be on the CPAP long the first time... If he does, then he is pretty much breaking records. The expectation is he goes on the CPAP, even for an hour or two, starts to struggle, and then has to be back on the machine. Then they would wait 24-48 hours and try the CPAP again. At least in that case, there was a time he was not on the machine, which is good. The smallest CPAP they have, size 0, is a little big for him. However, they are able to slowly dilate his nostrils to fit it... so for those that say he has my big nose... yeah, it'll be bigger, temporarily.
He is about due to remove his umbilical lines as well and to put in the PICC line. If you recall, the PICC line is just like your typical "IV" but a more long-term solution. Once they get his PICC line in, they will look at pushing him on the CPAP. For now, no CPAP so that way we can at least keep his breathing stable while they do the PICC line. The team that does it has been extremely busy with operating and dealing with other more urgent preemie care... it has been ordered so just a matter of when they get time away from the more critical babies.
If after 14 days (next Monday), he is still requiring the machine then there is a steroid they may give him to help his lungs. They gave Pru a steroid when she was in labor but instead of that particular one, they would give him hydrocortisone. The other steroid would be “like a bazooka to a mouse...” and can harm brain tissue. The hydrocortisone is more gentle. Let's just hope the indomethacin does its job. If that PDA is closed, then his respiratory should be dramatically improved and the conversations around a steroid are out of question. If the PDA remains, open, his respiratory can still get better, but it's just a longer road. They would also wait until he gets to be around 5 pounds and then send him to the University of Michigan cardiac hospital for a procedure to close the PDA (catheter... so much safer than opening him up). I know our son insisted on being a Michigan Man... He got that being born here. I hope that he doesn't think about visiting the UofM facilities just yet... at least not until I take him to his first Michigan football game.
The last two paragraphs are more the "what if" so hopefully we don't get to those points. However, if any of you are like me, you're wondering those things.
He is still off breast milk and that is only because of the indomethacin. His blood sugar is being maintained just fine... still no insulin. His bilirubin is good too as there has been no need for a biliblanket. This little man continues to surprise us and do great things. The next big wish list hurdle is for his lungs to improve so we can get him in the CPAP ASAP. Whether that is because he "feels like it" or the PDA closes, it doesn't matter to me. Just get on a CPAP and stay there as much as possible.
Thank you for the continued prayers and well wishes. #EthanStrong
The day started with the doctor checking him out and me informing her that I just finished reviewing his 6AM blood work and that his triglycerides appear steady and low so it would be appropriate to continue his lipids. She laughed and agreed. Haha!
Ethan’s blood gases (a measure of how well his lungs are working: Oxygenation and ventilation) have been looking pretty good so they lowered his Tidal Volume (amount of air they push to him per breath) down to 2.1. A value of 2.0 is basically no machine support. Additionally they have lowered his Rate (number of “forced breaths” per minute) from 60 to 40. He will have his ups and downs with his oxygen saturation but at least this is forcing him to learn how to use those lungs on his own without so much machine.
They just ran his gases again at 3PM and they were OK. They also checked his hematocrit and it came back low. This is the percent of red blood cells he has… being low means he is anemic. They are going to start a blood transfusion now and it will last a couple hours. I asked if there was any worry about this being his third transfusion (some other root cause??) and there is not. They think that it is from the amount of blood that they keep taking, therefore, no concerns of an underlying issue. Following the transfusion, he will get his CPAP. There is a pretty big leak with his tube now… his gases are OK… so may as well try the CPAP. Don’t be surprised if he has to be re-intubated (tube reinserted). As I have said before… any time off the machine is good. Maybe we’ll get lucky here and he’ll love the CPAP and not require the machine again.
They also tried the PICC line (a long-term IV that is a catheter) this afternoon but were not successful. The good news is that he took the abuse pretty well but of course, the bad news was that his artery was just a bit too small to get it in place. They tried in his left arm and there are other areas (leg and head) that they can attempt…. Next attempt could be tonight in one of those areas. While the Transport Unit (team that performs the procedure) was hoping for the first time, they still seemed hopeful that Ethan didn’t “crash” or have any immediate issues when they attempted. He took the poking like a champ. I spoke with the doctor a moment ago and she said they DO have a smaller gauge catheter…. just not in stock. Despite ordering it last week, apparently someone forgot the memo. She hopes it is here tomorrow…. If they can verify it will be here tomorrow then they will wait and try tomorrow… Otherwise, they may still try again tonight. With that said, worse case if they cannot get the PICC line through this method then there is a surgical method. Of course, like any surgery, you want to avoid if possible. However, it would still be very routine and straight forward… We hope that they can get the smaller catheter in tomorrow so they don’t have to keep unnecessarily poking our little guy.
The murmur appears to be maybe going away…. The doctor said it does sound less prevalent so it appears the indomethacin is doing its job. Even if the PDA remains a little open, that is OK. They do close on their own but he just needed that extra push to help with the oxygenation. I questioned why she said before “may as well do a round 2 and close ‘er up even if it lessens” and now she changed her mind. Her response was that since the meds, they have been able to reduce the amount of machine and his blood gases are improving. Before she did not anticipate it… so may as well stop the meds to avoid those unnecessary side effects. Pru is whining. Something about it being 9 degrees and -12 with wind chill. Her hands are chapped… blah blah blah. Maybe I’ll let her clean the car off in the mornings and THEN we’ll see how she feels. :-p
Other than that, she and I are doing much better. Each day that Ethan continues to not have a “down,” we are feeling more comfortable with the situation, relatively speaking. Thank you all for your continued support and prayers! #EthanStrong